TOTAL ANKLE REPLACEMENT
What is a total ankle replacement?
 Total ankle replacement is a type of joint replacement surgery. It’s also called ankle arthroplasty. It replaces damaged parts of the ankle with prosthetics (plastic and metal parts). These new parts work together and move like your natural joint. This treatment is usually only for people with ankle pain that doesn’t go away and affects their quality of life. Dr. Yorgason at Ortho Montana specializes in Total Ankle Replacement, using the Infinity Total Ankle System. You can hear about it from a local patient just like you:
Total ankle replacement is a type of joint replacement surgery. It’s also called ankle arthroplasty. It replaces damaged parts of the ankle with prosthetics (plastic and metal parts). These new parts work together and move like your natural joint. This treatment is usually only for people with ankle pain that doesn’t go away and affects their quality of life. Dr. Yorgason at Ortho Montana specializes in Total Ankle Replacement, using the Infinity Total Ankle System. You can hear about it from a local patient just like you:
Can my ankle be replaced safely?
Ankle replacement surgery has been an option for many years. Recent advancements in technology and techniques have made it the preferred option for treating patients with ankle arthritis.
Ankle replacement can take away the pain from the arthritis and preserve motion at the joint. This helps patients perform tasks such as walking on uneven ground and going up and down stairs. It also protects the other joints of the foot to help prevent them from getting arthritis.
What can ankle joint replacement treat?
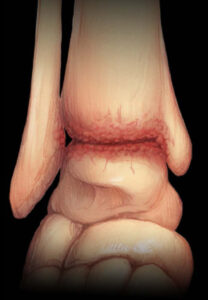 Total ankle replacement surgery usually treats ankle arthritis. Arthritis develops from changes to the cartilage which covers the bones of a joint. The cartilage becomes thinner and rougher. Ankle arthritis can happen with age, from general wear and tear. It may also come from repeated ankle injuries, ankle fractures or certain health conditions.
Total ankle replacement surgery usually treats ankle arthritis. Arthritis develops from changes to the cartilage which covers the bones of a joint. The cartilage becomes thinner and rougher. Ankle arthritis can happen with age, from general wear and tear. It may also come from repeated ankle injuries, ankle fractures or certain health conditions.
Common symptoms of ankle arthritis include:
Difficulty walking
Joint pain
Joint swelling
Joint stiffness
Many people find relief from ankle pain and other symptoms with basic treatments, often used together. Healthcare providers consider these treatments “conservative therapies.” They may include medications, physical therapy, steroid injections or orthotics (special shoe inserts or devices, like braces, to relieve pain). Sometimes, though, severe ankle arthritis requires more targeted treatment. When that happens, a healthcare provider may suggest total ankle replacement.
Ankle joint anatomy and arthritis
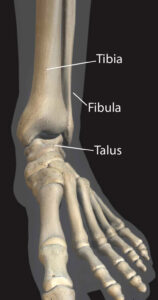 The ankle (known by doctors as the tibiotalar joint) is a complex joint that allows your foot to rotate and pivot in relation to your leg. Three separate bones meet to form the ankle joint. These are the:
The ankle (known by doctors as the tibiotalar joint) is a complex joint that allows your foot to rotate and pivot in relation to your leg. Three separate bones meet to form the ankle joint. These are the:
Tibia (the large bone in your leg)
Fibula (the smaller bone on the outside part of your leg)
Talus
Cartilage (cushioning) covers the ends of these bones to allow them to glide together smoothly. If the cartilage in the ankle becomes damaged or wears down due to injury or disease, the bone surfaces will rub each other during movement. This causes osteoarthritis (joint inflammation, or pain and swelling) in the ankle. Over time, the bone-on-bone grinding of osteoarthritis can wear away the bone surfaces, causing bone spurs and stiffness in the joint.
What is actually replaced in a total ankle replacement?
The surface of the tibia and the surface of the talus that make up the ankle joint is removed. In its place, metal pieces are inserted into the bone. Then, a plastic insert is attached to the metal piece on the tibia. In a replacement, the metal piece on the talus will rub against the plastic piece attached to the tibial implant. This takes away the pain of the ankle arthritis and preserves the motion in the joint.
Who should not have ankle replacement surgery?
Ankle replacement is not the best option for every person with ankle arthritis. It may not provide a good fit for you if your ankles are severely deformed or unstable. Similarly, healthcare providers may not recommend replacement for people with certain medical conditions:
- Bone infections.
- Circulatory problems.
- Diabetes.
- Neuropathy.
- Obesity.
The first step is to see a healthcare provider who will perform a physical exam and x-rays to determine if you are a candidate for an ankle replacement. Ankle replacement is not the only type of ankle surgery. If ankle replacement isn’t the right procedure for you, other possibilities include: ankle fusion or ankle arthroscopy.
How do I prepare for total ankle arthroplasty?
It’s important to go into surgery and rehabilitation (recovery) with realistic expectations. Talk to members of your care team about how to get ready for the procedure. Knowing what to expect can help you prepare for challenges and make plans for recovery. Before surgery, your team may recommend that you:
- Start physical therapy.
- Stop smoking.
- Stop taking certain medications.
Discuss what recovery might look like with your family and friends. You’ll have trouble walking after your ankle replacement. Be sure to make a plan for accomplishing daily tasks. You may need help grocery shopping, getting up and down stairs, or caring for a pet.
What happens during total ankle joint replacement?
Only a highly skilled orthopedic surgeon should perform total ankle joint replacement. The surgeon works with an anesthesiologist, nurses and other healthcare providers. Together, the team will:
- Give general anesthesia or a spinal block.
- Make an incision in the front of your ankle.
- Remove the degenerated (worn-down) bone and cartilage.
- Prepare the joint surface for the new prosthetic pieces.
- Insert the pieces and check range of motion in the joint.
- Perform other procedures to make sure proper ankle and foot alignment.
Total ankle replacement is typically an inpatient procedure, but you usually only spend one night in the hospital after surgery. Some patients may be candidates for outpatient total ankle replacement surgery.
What are the risks and benefits of ankle replacement?
An ankle replacement helps you regain strength and stability in your ankle. The treatment also preserves range of motion. The replacement parts articulate, or move together, like your natural joint. This flexibility can allow you to walk normally, with less pain, and return to a more active lifestyle.
Often, ankle replacement is preferable to ankle fusion (arthrodesis). Fusion surgery permanently joins the ankle bones together, limiting range of motion. This loss of flexibility can affect the way you walk or cause arthritis to develop in other joints. Talk to your provider about which procedure — ankle replacement or ankle fusion — best fits your unique needs.
Although rare, ankle surgery can lead to complications. Possible risks of ankle replacement include:
- Blood clots.
- Infection.
- Loosening of replacement parts, requiring a procedure to repair.
- Nerve or blood vessel damage.
- Problems healing the incision.
- Wearing down of metal and plastic replacement parts over time.
How long is recovery after ankle arthroplasty?
Recovery from ankle arthroplasty can take anywhere from 3 to 12 months. Most people use crutches, a walker or a knee scooter while wearing cast. The cast keeps the ankle immobilized to allow for healing. During this time, your healthcare provider will ask you to take medications to prevent blood clots.
Physical therapy usually starts around 8 weeks after surgery and can help you regain mobility in your ankle. Rehabilitation may include:
- Gait training to help you stand and walk.
- Massage to decrease swelling.
- Strengthening exercises.
- Stretches for range of motion and flexibility.
- Weight-bearing activities that get harder over time.
Your healthcare provider may recommend coming in for scans and follow-up visits after surgery. This extra care can ensure your ankle heals properly.
When should I call a doctor after a total ankle replacement?
Contact a healthcare provider if you experience any of the following complications after surgery:
- Worsening ankle or foot swelling.
- Fever.
- Pus or a lot of blood draining from the incision.
- Signs of infection.
You can reduce your risk of complications after surgery by eating a healthy diet and not smoking. Also make sure to follow all medical instructions. Some people face an increased risk of developing problems after ankle surgery. This group includes people who smoke or who have diabetes or an autoimmune disorder.
Ankle arthritis is a common complaint. Rest, ice, elevation and other basic treatments can usually relieve joint stiffness and pain. Surgery to treat ankle arthritis may provide an option when other therapies don’t work. Avoid smoking, maintain a healthy body weight and get plenty of low-impact exercise.
ANKLE & ACHILLES TENDONITIS
Achilles tendonitis is an inflammation of the Achilles tendon, the strong band of tissue that connects the calf muscle to the heel. This condition occurs when excessive stress is put on the tendon. Achilles tendonitis is usually a painful but short-lived condition.
WHAT CAUSES ACHILLES TENDONITIS?
Achilles tendonitis is usually caused by excessive or repetitive strain on the tendon. It is frequently found in athletes who suddenly increase their activity level, or in middle-aged individuals who exercise intensely but irregularly. Older individuals are at increased risk of injuring the tendon because tendons weaken during normal aging. Movements that may put strain on the Achilles tendon include walking, running, jumping or pushing up onto the toes.
RISK FACTORS FOR DEVELOPING ACHILLES TENDONITIS
Apart from age and improper preparation for exercise, other risk factors for Achilles tendonitis include:
- Being male, being obese
- Having flat feet or tight calf muscles
- Wearing non-supportive footwear
- Exercising in very cold weather or on hilly terrain
- Having diabetes or hypertension
Taking certain antibiotics, known as fluoroquinolones, such as Cipro and Levaquin, also puts individuals at greater risk of developing Achilles tendonitis.
WHAT ARE THE SYMPTOMS OF ACHILLES TENDONITIS?
Typically, the pain of Achilles tendonitis initially manifests after engaging in a sports activity as a mild ache in the calf or above the heel. Other symptoms may include:
- Increased pain after running or climbing stairs
- Pain when walking
- General tenderness and swelling at the site
- Stiffness or tenderness upon awakening
- Lessening of pain with mild activity
If a patient experiences severe pain or disability in the region of the Achilles tendon, a ruptured tendon should be suspected and medical attention should be sought immediately.
DIAGNOSING ACHILLES TENDONITIS
Achilles tendonitis is usually diagnosed through a combination of physical examination, including an assessment of flexibility, range of motion, reflexes, inflammation and alignment at the injury site, and one or more of the following imaging tests:
- X-rays
- MRI scan
- Ultrasound
The chief purpose of these imaging tests is to rule out the possibility of a tendon rupture, a more serious injury that requires surgical intervention.
TREATMENT OPTIONS FOR ACHILLES TENDONITIS
As with most injuries, conservative methods of treatment are normally tried first, but the initial treatment will depend, to some extent, on the patient’s level of pain and dysfunction.
HOME CARE
Tendonitis usually responds well to self-care measures, including rest, ice application, and elevation of the affected area, in combination with over-the-counter pain and anti-inflammatory medication.
ASSISTIVE DEVICES AND ORTHOTICS
In order to relieve pain and accelerate healing by taking weight off the injured area, assistive devices, such as, walking boots, crutches or canes may be recommended and prescribed. Orthotics, or shoe inserts, may also be suggested to provide a cushion that diminishes pressure exerted on the Achilles tendon.
PRESCRIBED MEDICATIONS
When over-the-counter medications are insufficient, the doctor may prescribe stronger analgesics or anti-inflammatories.
PHYSICAL THERAPY
Physical therapy may be advised as an alternative method of treatment. Physical therapists are trained to instruct and assist in exercises the patient can use to stretch, strengthen and heal not only the Achilles tendon, but the adjacent, supportive region. They may also use laser, ultrasound and electrical stimulation as part of the rehabilitative process.
SURGERY
If diagnostic tests have shown that the Achilles tendon is torn or ruptured, or if the patient doesn’t show marked improvement after several months of conservative treatment, surgical repair of the Achilles tendon may be necessary.
If surgical intervention is necessary, most patients will require physical therapy after the operation to regain maximum strength and flexibility.
CAN ACHILLES TENDONITIS BE PREVENTED?
Most cases of Achilles tendonitis can be prevented by beginning an exercise regimen slowly, with preparation, and by increasing an exercise program gradually and with care.
WHAT HAPPENS IF ACHILLES TENDONITIS IS LEFT UNTREATED?
If not treated, however, Achilles tendonitis can increase the risk of Achilles tendon rupture, a serious injury requiring immediate medical attention.
FOOT SPRAINS AND STRAINS
Both foot sprains and foot strains are very common injuries, occurring as a result of sports accidents, falls, or other traumas. The difference between the two types of injuries is that sprains affect the ligaments, the thick strands of cartilage attaching one bone to another, and strains affect the muscles or the tendons, thick bands attaching muscle to bone. In both cases, the patient with the injury usually experiences pain (particularly upon movement), swelling, tenderness, bruising, weakness or muscle spasms. Foot sprains, the more serious injury, may also cause possible instability of the joint, most frequently the ankle. Depending on where on the foot the injury occurs, patients may be unable to bear weight until healing takes place.
CAUSES OF FOOT SPRAINS AND STRAINS
Typically, foot sprains occur in the ankle or midfoot as an abnormal twisting during an athletic event or accident. When a sprain occurs in the big toe, rather than midfoot, it is referred to as turf toe. This injury is the result of an awkward twisting or hyperextension of the affected appendage. Foot strains, on the other hand, happen as the result of a sudden tear or pull of the affected muscle, usually because of overstretching or over contraction.
DIAGNOSIS OF FOOT SPRAINS AND STRAINS
Foot sprains and strains are routinely diagnosed through physical examination of the patient and an evaluation of the circumstances of the injury as well as its resulting symptoms. X-rays may also be taken to confirm the diagnosis and to rule out other problems, such as bone fractures. When diagnosed, both sprains and strains are graded as I, II or III, depending on severity of injury, pain level and lack of function. For both sprains and strains, the categories are designated mild, moderate and severe.
TREATMENT OF FOOT SPRAINS AND STRAINS
Mild foot sprains and strains can normally be successfully treated through the usual remedies of rest, ice, compression and elevation (RICE). Over-the-counter anti-inflammatory medication is typically administered to reduce swelling and alleviate pain. In some circumstances, mild stretching exercises may be helpful.
While severe sprains may require complete immobilization with a cast, with lesser sprains and strains the patient may be able to walk with a bandage or brace, aided by a cane, or may not require any assistance. Most patients heal gradually from mild or moderate sprains in approximately 2 to 8 weeks, depending on the severity of the injury.
In the case of severe sprains or strains, a surgical repair may be necessary, in which case the recovery period may stretch to 3 months. After immobilization for a lesser injury or after surgery for a more severe one, a period of physical rehabilitation is necessary.
CAVOVARUS FOOT DEFORMITY
A cavovarus foot deformity is a condition in which the foot has an abnormally high arch and the heel slants inward. This condition places more weight than normal on the ball and heel of the foot during walking or standing, causing pain and instability. Usually present in childhood and often affecting both feet, a cavovarus foot deformity typically worsens over time and frequently requires surgical repair.
CAUSES OF CAVOVARUS FOOT DEFORMITY
A cavovarus foot deformity may occur as a congenital defect, sometimes combined with another foot abnormality such as a club foot. The anomaly may also be the result of:
- Neurological disorders like cerebral palsy or muscular dystrophy
- Charcot-Marie Tooth disease, a hereditary neuropathy
- Stroke or spinal injury
- Spinal tumor
- Traumatic injury, such as a severe fracture or burn
A certain number of cases are idiopathic, meaning they occur for unknown reasons.
SYMPTOMS OF CAVOVARUS FOOT DEFORMITY
The exceptionally high arches of a cavovarus foot cause abnormal pressure on the bones of the forefoot, known as the metatarsals, which can result in pain, especially on the heel, ball or side of the foot. The high arches also effectively shorten the foot, making it problematic for patients with this condition to find shoes that fit properly.
Apart from the noticeably high arch of the foot and the concomitant discomfort it produces, other symptoms of the condition may include:
- Foot weakness and fatigue
- Hammertoes
- Claw toes
- Foot instability
- Calluses
Because of the abnormal pressure on the foot and ankle, patients with cavovarus foot deformity are also prone to ankle sprains and stress fractures.
DIAGNOSIS OF CAVOVARUS FOOT DEFORMITY
In order to diagnose a cavovarus foot deformity, a full evaluation is performed, including medical history and physical examination. The patient will be examined in both a standing position and a supine posture (lying down). In addition, the patient’s gait will be carefully observed. In many cases, X-rays, muscle tests, MRI and CT scans may also be administered.
TREATMENT OF CAVOVARUS FOOT DEFORMITY
There are several treatment options for a cavovarus foot deformity, depending on the severity of the individual case. The goal of all such treatments is to relieve pain and improve stability. When the condition is mild, patients may achieve sufficient pain relief and support through the use of orthotics, orthopedic shoes, foot or ankle braces. If the condition does not improve or worsens, however, surgical intervention may be necessary.
The three surgical techniques employed to correct the muscle imbalance of cavovarus foot deformity are osteotomy (removal or realignment of a bone), tendon transfer, or arthrodesis (bone fusion).
FLAT FEET
WHAT ARE FLAT FEET?
Flat feet (pes planus) are extremely common. While usually just a normal anatomical variation that does not result in any serious difficulties, this condition, which causes the feet to lean inward, or pronate, can cause problems over time.
Infant’s feet are naturally flat because of the pad of “baby fat” at the instep. As they grow and begin to walk, their feet normally develop arches. For some children, this does not happen and their feet remain flatter than average. While this condition is usually inherited, there are many individuals who have normal arches as children and young adults but develop flat feet, or “fallen arches,” over time. These individuals are said to have acquired flat foot deformity (AFFD).
TYPES OF FLAT FEET
There are two basic types of flat feet: rigid and supple. If the medial longitudinal arch (MLA) is not visible whether the patient is either seated of standing, the condition is called rigid MLA. If, on the other hand, the MLA is present when the patient is seated or standing up on the toes, disappearing only when the patient stands, the condition is known as supple MLA. The latter condition is less serious and can most often be alleviated with the use of arch supports or orthotics.
SYMPTOMS OF FLAT FEET
Many individuals with flat feet have no discomfort at all because of the condition, but some may experience foot fatigue and pain, Some, particularly as they age, develop pain in the heel or arch area, or swelling along the inside of the ankle.
When the condition of an individual with flat feet deteriorates, the person may suffer from pain or aching not only in the foot, but in the ankle, knee, or back. It is also common for such people to develop bunions, arthritis, or another foot or ankle deformity. In such cases, medical intervention may become necessary.
DIAGNOSIS OF FLAT FEET
While flat feet are diagnosable through simple physical examination, diagnostic imaging tests may be used to detect anatomical abnormalities, soft tissue injuries, such as those affecting the tendons, and any arthritis that has developed in the area. Such imaging tests include:
- X-rays
- CT scan
- Ultrasound scan
- MRI scan
These tests are often necessary to determine whether treatment is necessary and, if so, what type.
RISK FACTORS FOR PROBLEMATIC FLAT FEET
Apart from heredity, there are several risk factors that predispose certain individuals to developing flat feet that are troublesome and may require medical intervention. These risk factors include wear and tear due to aging or obesity, disease conditions such as rheumatoid arthritis, traumatic injuries, and dysfunctions of tendons or ligaments. The most serious of the latter is posterior tibial tendon dysfunction in which the primary tendon that supports the arch gradually becomes lax.
IS THERE TREATMENT FOR FLAT FEET?
For children with flat feet that trouble them, walking barefoot, particularly on soft terrain like sand, is recommended. There is some evidence that this may assist them in developing normal arches. Wearing supportive shoes and orthotic devices can be helpful to individuals of any age.
Other treatments for pain or fatigue resulting from flat feet include over-the-counter anti-inflammatory medication, applications of ice packs, stretching exercises and physical therapy.
When flat feet have resulted in, or a have been caused by, more serious foot abnormalities, such as bone spurs or tendon ruptures, surgery may be required. Depending on the patient’s condition, this may involve removing a bone spur, repairing a tendon or ligament, or fusing one or more bones of the foot.
POSTERIOR TIBIAL TENDON DYSFUNCTION
Posterior tibial tendon dysfunction occurs when the posterior tibial tendon of the foot becomes torn or inflamed. Commonly referred to as flat foot, this condition often results in the inability to provide support for the arch of the foot. The posterior tibial tendon is the tendon that attaches the calf muscle to the bones on the inside of the foot and ankle, and is responsible for creating the arch in the feet. This tendon provides the support that normally holds up the arch of the foot while walking. As the tibial tendon tears, individuals often experience pain as the foot gradually rolls inward and flattens. Over time, the supporting ligaments in the foot begin to stretch and tear as well.
CAUSES OF POSTERIOR TIBIAL TENDON DYSFUNCTION
Posterior tibial tendon dysfunction may be a condition that some people are born with. Other causes may include:
- Stretched or torn tendons
- Nerve problems
- Fractured or dislocated bones in the leg or foot
Posterior tibial tendon dysfunction often occurs in athletes such as basketball and tennis players who may have tears in this tendon from repetitive use. This condition is also more common in women, people who are obese and people with diabetes.
SYMPTOMS OF POSTERIOR TIBIAL TENDON DYSFUNCTION
Some people with this condition may not experience any symptoms at all, however, others may experience:
- Pain along the inside of the foot and ankle
- Swelling
- Limited flexibility
- Pain that intensifies with activity
- Pain on the outside of the ankle
The shape of the foot may also change in individuals with posterior tibial tendon dysfunction, as the heel may tilt outwards and the ankle may roll inwards,as the arch of the foot collapses.
DIAGNOSIS OF POSTERIOR TIBIAL TENDON DYSFUNCTION
Tibial tendon dysfunction is diagnosed through a physical examination and a review of symptoms as well as diagnostic tests that may include X-rays, CT scans or MRI scans.
TREATMENT OF POSTERIOR TIBIAL TENDON DYSFUNCTION
Initial treatment for posterior tibial tendon dysfunction may include conservative methods that may include:
- Rest
- Applying ice to the affected area
- Anti-inflammatory medication
- Immobilization through a short cast or walking boot
- Physical therapy
Additional treatment for this condition may also include orthotic devices or braces to support the joints of the foot. In severe cases that do not respond to conservative methods,surgery may be required to cut or realign the bones and correct the deformity. Surgery often involves an osteotomy, which cuts and shifts the heel bone in order to transfer another tendon to be used in place of the torn tibial tendon. Other surgical methods may also include lengthening of the achilles tendon or a fusion of the joints in the back of the foot. Most patients have successful results from surgery.
Left untreated, posterior tibial tendon dysfunction may cause arthritis in the foot and ankle and limitations to physical activity.
LISFRANC INJURY
A Lisfranc injury is a trauma to the midfoot where the Lisfranc (tarsometatarsal) joint is located. This joint enables the articulation of the middle of the foot. A Lisfranc injury may vary in severity, involving a sprain, a torn ligament, a fracture or a dislocation. Lisfranc injuries are relatively rare and frequently misdiagnosed. Lisfranc injuries occur for a number of reasons, all of which involve suffering a crushing blow, falling or twisting the foot. Causes of Lisfranc injuries may include vehicular collisions, falls and sports injuries.
SYMPTOMS OF LISFRANC INJURY
The symptoms of a Lisfranc injury are pain, swelling and bruising in the middle of the foot, as well as difficulty standing or walking. When such symptoms present, it is important to seek immediate medical care because of the potential difficulty in diagnosing the condition and the possibility that, without prompt treatment, proper healing may not take place.
DIAGNOSIS OF LISFRANC INJURY
The Lisfranc joint and the injury are named for the Napoleonic field surgeon who tended a soldier with a severe injury to that region. Lisfranc injury should be suspected when there is midfoot swelling and when the patient is unable to put weight on the joint. Sometimes such an injury takes place in conjunction with the fracture of a toe or other small bone in the foot, so when foot injuries occur, it is important that the entire foot be carefully examined. The physical examination for a Lisfranc injury includes rotating the foot in circles. X-rays will also be taken to confirm the type of Lisfranc injury, its precise location and severity.
TREATMENT OF LISFRANC INJURY
Treatment for a Lisfranc injury depends on the severity of the injury, but may include immobilizing the foot, casting or surgery to secure the bones in place with pins, wires or screws while they heal. Physical therapy may be needed to restore proper function to the foot after it heals. Proper treatment for a Lisfranc fracture is critical, as this area bears most of the weight of the foot and is essential in allowing the patient to walk properly and painlessly.
TURF TOE
Turf toe, which is a sprain of the soft tissue in the main joint in the big toe, is a common sports injury. Although it derives its name from the fact that it is frequently suffered by football players who play on artificial turf, it is also a common ailment of wrestlers, gymnasts, soccer players and dancers. Turf toe is usually caused by jamming or pushing the big toe while running or jumping, which results in swelling, pain and limited joint movement at the base of the toe. Typically, the injury to the toe is sudden (a “pop” may be felt), although it sometimes develops gradually after repeated trauma. Turf toe is diagnosed by physical examination.
TREATMENT OF TURF TOE
At-home treatment using RICE (rest, ice, compression, elevation) is often sufficient; it promotes healing, reduces inflammation and protects the foot from further injury. Over-the-counter anti-inflammatory medications are usually recommended until the pain and swelling subside.
After the approximately 2 to 3 weeks that turf toe takes to heal, physical therapy may be required, particularly for athletes, to regain strength and mobility. The only time surgery is necessary for turf toe is if the bone is chipped or the ligament is completely torn.
COMPLICATIONS OF TURF TOE
Apart from being extremely painful, if left untreated turf toe can lead to instability and, even, dislocation of the joint, which, in turn, can cause degenerative arthritis of the big toe, a condition known as hallux rigidus. The risk of developing turf toe is reduced by wearing well-fitting, supportive footwear with stiff soles and, if necessary, appropriate orthotics.
